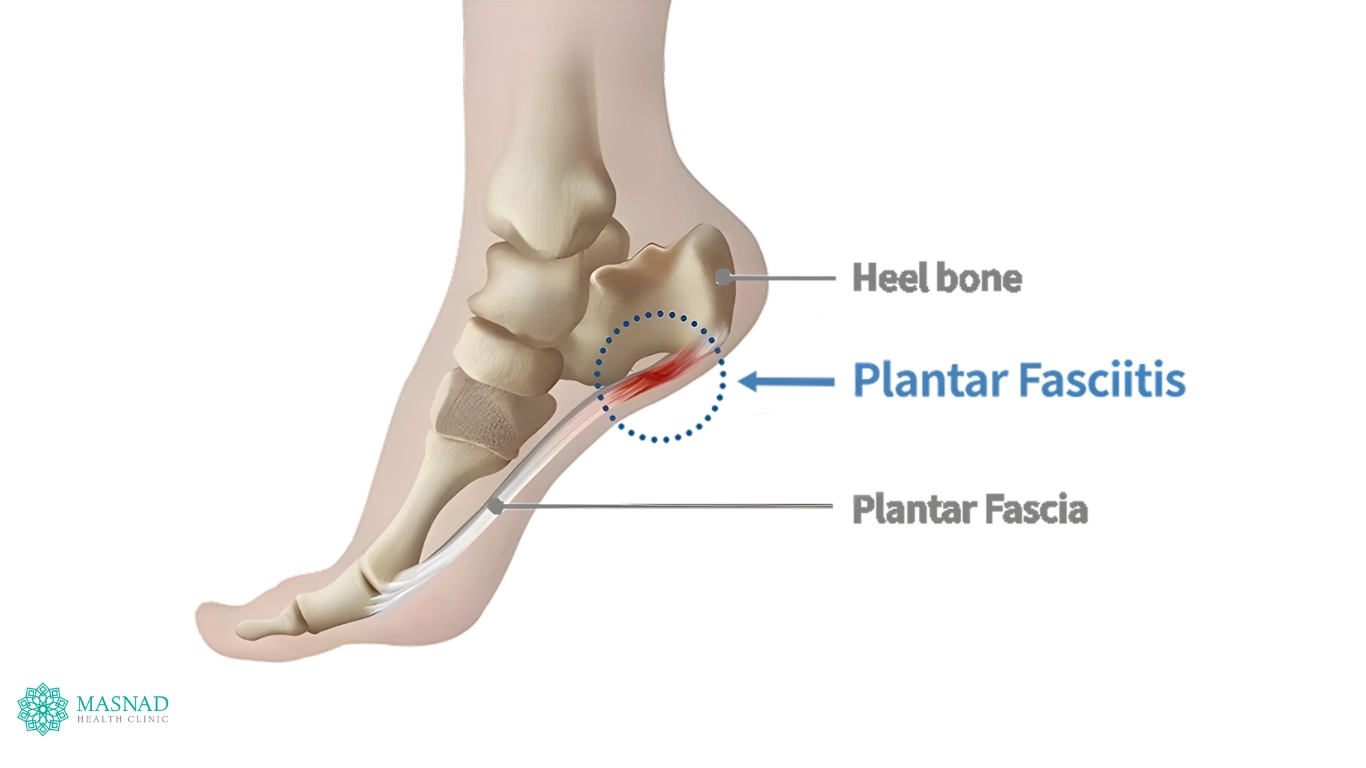
The plantar fascia is a thick, fibrous band of tissue that runs along the bottom of your foot – connecting your heel bone to your toes. Its main role is to support your foot’s arch and absorb shock as you walk, run, or stand.
Over time, repeated stress or overuse can cause tiny tears in this tissue. When these stresses exceed the fascia’s ability to repair itself, degeneration occurs, leading to pain when pressure is placed on the heel – especially with your first few steps in the morning.
This condition is called Plantar Fasciopathy – also commonly known as Plantar Fasciitis. While the term “fasciitis” implies inflammation, Plantar Fasciopathy is actually more of a degenerative condition.
It can be progressive, and although it sometimes resolves on its own, without treatment it may take up to two years to go away – and can be extremely painful during that time.