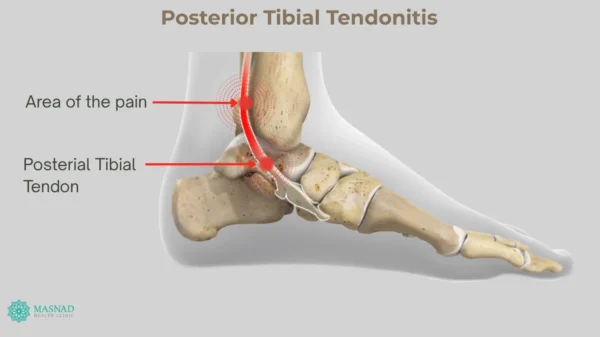
The tibialis posterior muscle sits deep in the lower leg, just inside the shin. Its tendon travels downwards, curves behind the inner ankle (medial malleolus), and attaches into the base of the foot’s arch. The tendon is crucial for foot and ankle movement – it helps you move your foot downward and inward (plantar-flexion & inversion) and supports the arch of your foot.
When this tendon is put under too much strain, or repeatedly stressed, it may develop degeneration, micro-tears, swelling and impaired function. That condition is known as tibialis posterior tendinopathy. Over time, if left untreated, it may weaken and elongate, reducing its ability to support the arch and potentially contributing to flat-foot deformity.