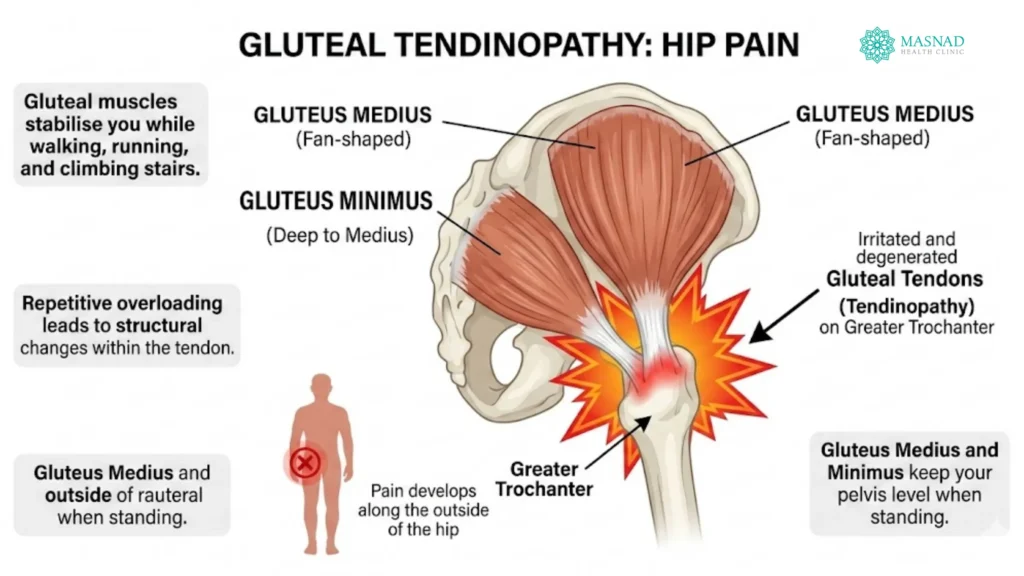
What is Gluteal Tendinopathy?
Gluteal Tendinopathy is a condition involving irritation and degeneration of the gluteal tendons on the outer side of the hip.
Tendons connect muscles to bone. When they are repeatedly placed under more load than they can tolerate, they may fail to heal properly. This leads to structural changes within the tendon – known as a tendinopathy.
In this condition, the affected tendons are usually those of the gluteus medius and gluteus minimus muscles. These muscles attach from the pelvis and connect to the outer part of the upper thigh bone, called the greater trochanter.
The gluteal muscles:
- Keep your pelvis level when standing
- Control hip movement
- Stabilise you while walking and running
- Help with stairs and single-leg activities
When these tendons become irritated, pain develops along the outside of the hip.