Lumbar facet joint arthropathy is a disease that affects the joints of the spine and causes the cartilage at such joints to be disintegrated; resulting in impaired joint movement and inflammation of the surrounding tissue. It is a degenerative disease.
Lumbar Facet Joint Arthropathy
What is Lumbar Facet Joint Arthropathy?
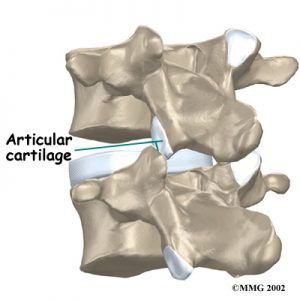
What Causes It?
Joints enable us to move and carry out activities with ease. However, the cartilages at these joints in the spine wear and tear with time. This leads to the bone to come in direct contact with bone. When this happens, the affected person may experience lower back pain and back stiffness. Other causes include a lifestyle of repetitive bending and twisting movements, poor posture, sedentary lifestyle, sudden fall and it can be hereditary.
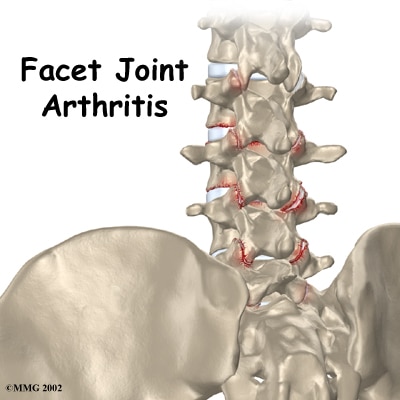
Symptoms
A person with facet joint arthropathy may experience one or more of the following:
- Dull pain across the back of the patient.
- Impaired flexibility and motion of the back.
- Sudden pain when performing the activities that caused the disease.
- Muscle spasm around the affected joints and referral pain in the buttock or lower limb of the affected side.
- Difficulty sitting for prolonged periods of time.
Do I Need A Scan?
A Physiotherapist or Doctor will determine if you need a scan and what type of scan you require. The Physiotherapist employs special skills in examining the spine, after which they will determine if an X-ray, MRI or a CT scan is required for further investigation.
Initial Management
Rest to avoid further aggravation and to allow the inflammation in the region to settle. This means that the patient should not engage in any activity that results in pain in the affected area, such as twisting or bending movements of the lower back. Use of Ice and anti-inflammatory medication can be used to alleviate the pain. Lower back supports can also be used to reduce pressure on the facet joints. Please note that lower back supports are advised in initial management and not for prolonged use. Extensive use of lower back supports will cause your lower back muscles to weaken as they don’t need to work as much with the brace on. This will lead to more pressure on the facet joints and increased reliance on the back support, therefore hindering a full recovery.
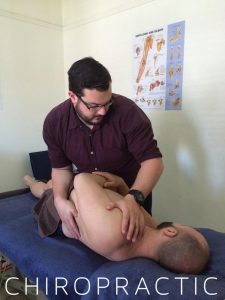
Treatment
In either mild or severe cases the best way to treat lumbar facet joint arthropathy is to see a Physiotherapist or Chiropractor. The specialist carries out gentle hands-on procedures to ensure each joint is moving well and then proceeds to prescribe an exercise plan to maintain good joint movement and to strengthen the muscles of the lower back. Each exercise program is tailor made to meet the needs of each patient.
Medication
Your Doctor may prescribe one or more of the following medications:
- Pain relief medication: this may vary from over the counter to stronger medication depending on the severity/persistence of the pain.
- Anti-inflammatory medication to reduce inflammation of the affected area.
- Muscle relaxers this may be used in the case of acute muscle spasm.
- Cortisone injections into the facet joint may result in relief and reduction of localised inflammation. This is usually done with the aid of Image guidance due to the location of the facets; which is deep in the back and proceeded by Para-spinal muscles.
- In the case of a non-responsive condition, surgery may be indicated.
Physiotherapy Interventions
Some of these may be employed:
- Manual Therapeutic Technique; Gentle hands-on procedure that aligns and improves mobility of the affected joints.
- Therapeutic Exercises: highly effective for low back pain treatment.
- Neuromuscular re-education(NMR); Teaching the patient how best to manage and carry out daily activates such as; sleep, sitting and other forms of movement. This ensures lesser pain, faster recovery and prevents deterioration of the patient’s condition.
- Exercise plan: this includes various strengthening, stretching and stabilizing exercises.
- Others include: hydrotherapy, electrotherapy, cupping, dry needling, use of a back brace and lumbar rolls.
Exercises
The following are common exercises prescribed as part of the regimen for low back pain. They should be carried out three times daily after being discussed with your Physiotherapist. The Physiotherapist will guide you when to begin these initial exercises and when to progress your rehabilitation program.
When carrying out these exercises remember it is okay to experience a little discomfort, but if the pain is severe, then the routine must be discontinued completely and consult with your Physiotherapist.
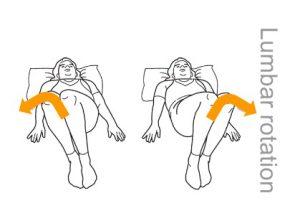
Lumbar Rotation
Lying flat on the back with knees bent upwards and feet firmly on the ground, move knees from side to side for 30-45 seconds.
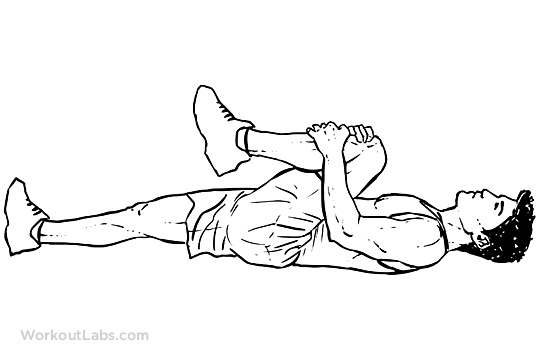
Knee To Chest
lying flat on a surface, extend one leg straight and pull the other knee to your chest and hold for 3-5 seconds, Switch sides. Repeat this procedure for as much as 8 to 10 times as long as there is no severe pain. This stretches the buttocks and lower back of the bent leg and the hip flexor of the straight leg.
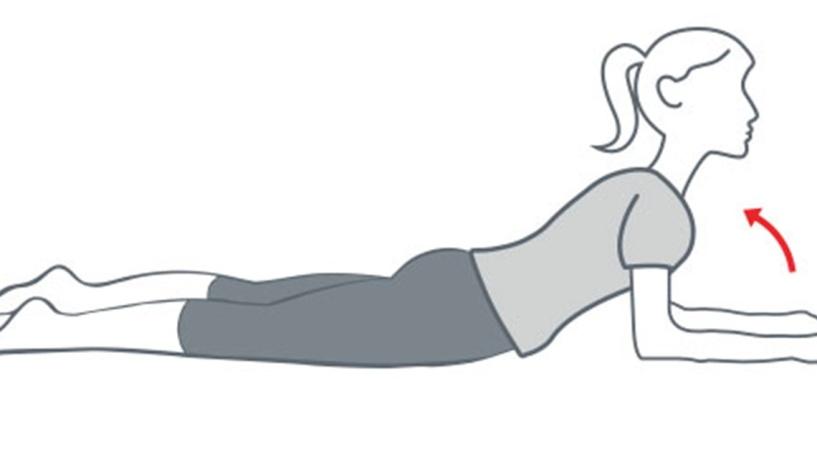
Elbow Prop
lying flat on a surface, gently raise your head up and hold the position for about 3-5 seconds then return to lying flat. Repeat this procedure for as much as 8 to 10 times as long as there is no severe pain
Tips & Tricks For Managing Daily Activities
- If you need to carry heavy loads, divide it into several sets of lighter portions
- Go for short walks at intervals to avoid sitting for a long time.
- Observe good posture always, i.e. when sitting, standing and walking.
- Keep things on surfaces that do not require you to bend, stretch or twist when you need to access them.
When Do I Get Better?
You should notice an improvement in your movement, reduction in pain and/or increased function with daily tasks 24-48 hours after your first visit with a Physiotherapist or Chiropractor. However, in most cases it takes 4-12 weeks for a full recovery but this varies proportionally to the severity of the condition and how compliant the patient is with their exercise program and their therapeutic appointments.
Prevention
Low back pain and back stiffness caused by facet disease can be prevented by engaging in exercises that enhance blood circulation, flexibility and strength. A sedentary lifestyle leads to weight increase and consequently more pressure on the spine. It can also be prevented by:
- Maintaining a healthy diet.
- Managing stress with yoga and meditation.
- Avoiding substances that dry out the joints; such as alcohol and tobacco.
Take Home Message
Do not delay seeing a Physiotherapist or Doctor.
Cease all aggravating activities but endeavor to be as active as you can.
Maintain good posture when sitting, standing or walking.

New Client Offer - 10% OFF
Are you in pain? Not sure if we can help you?
Book your initial appointment and receive 10% off any service!