This term refers to the general degeneration of the spine and the shock-absorbing intervertebral discs. It can strike the neck, the middle back, or the lower back. Thus, we have cervical (neck) spondylosis, thoracic (mid-back) spondylosis, and lumbar (lower back) spondylosis.
Spondylosis
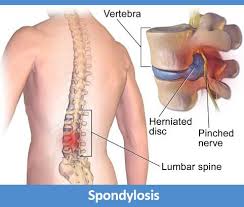
What is Spondylosis?
Causes
While the wear and tear associated with natural life and age are the primary causes of spondylosis some factors can exacerbate or even worsen the disease.
- Malnutrition
- Excessive use of alcohol and/ or smoking
- Genetic predisposition, a family history of back pain, or congenital spine abnormalities
- Lack of exercise
- Unexpected or sudden trauma or injuries, like those which can happen in hard falls, high-impact sports, motor vehicle accidents, or during manual labor
- Obesity
- Conditions like bone spurs, herniated discs, degenerative disc disease, or facet joint osteoarthritis
Symptoms
There are a variety of symptoms which can arise. Take note of these general symptoms:
- Pinched Nerves
- Headaches
- Herniated Discs
- Sciatica
- Lower Or Middle Back Pain
- Limited Range Of Motion
- Numbness And Weakness In Affected Areas
- Tingling, Pins-And-Needles Sensation In The Affected Area
- Trouble Maintaining Balance, Inability To Perform Daily Activities Without Pain Or Discomfort
Diagnosis & Treatment
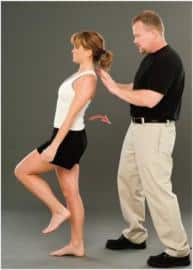
X-rays can confirm a diagnosis. One test that is helpful, although not conclusive, is the one-legged hyperextension maneuver. For this, the patient stands on one leg in a position which hyperextends the lower back. This is repeated on the opposite side. If there is pain, it can indicate spondylosis.
Surgery
There are two procedures which are done as part of one surgery:
The first is decompressive laminectomy, and this reduces inflammation and irritation in the affected area. However, it also increases spinal instability.
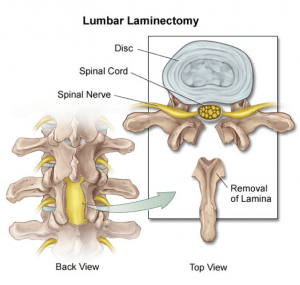
The second is a spinal fusion, to stabilize the affected area.
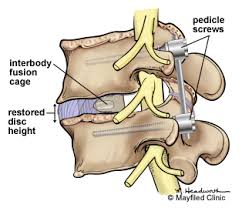
Be aware that you may need to stay in the hospital for as long as 5 days, or you may be lucky enough to leave after one day. Whatever the length of your stay, you won’t have to spend all that time lying down. In fact, getting up and walking around as soon as possible after surgery is encouraged because it cuts down on the chances of post-operative complications such as pneumonia. This gentle activity is easy on the spine and can even enhance healing. After leaving the hospital, you may still have to wait between 6 to 12 weeks before your doctor thinks it is safe for you to begin rehabilitation. Note that depending on how complicated the fusion surgery was (perhaps a multilevel fusion), you may have to restrict your activity level after you pass the rehabilitation stage. Generally speaking, though, this is not necessary if the surgery wasn’t very complicated at all.
Treatment
Treatment is usually a combination of bracing, pain or anti-inflammatory medications as needed (both prescription and non-prescription medications can help), gentle stretching which progresses to additional, harder stretching over time, and exercise. The latter must be controlled, and gradually built up over time. For those rare cases where it has been determined that there are neurological components involved or the condition is not improving, surgery may be required.
Prognosis
In general, prognosis is favorable. Many who have spondylosis may not even present symptoms. Of those who do have pain in the neck and/or back, there is improvement within a few weeks of the onset of symptoms. On rare occasions, chronic pain may result from spondylosis.
Prevention
Because spondylosis is a degenerative disease, and there is no cure, there’s no way to prevent it. (don’t you think this sentence is too decisive? “Because spondylosis is degenerative disease the prevention is the key. Regular exercises can help to prevent spondylosis which include walking, swimming, specific rehabilitation exercises focusing on stability and mobility of spine that can be prescribed by physiotherapist or chiropractors.) If it is detected early enough, that allowed you more time to consult with a doctor to decide on the best course of action. As with all diseases, early detection is best.

New Client Offer - 10% OFF
Are you in pain? Not sure if we can help you?
Book your initial appointment and receive 10% off any service!