Frozen shoulder, also known as adhesive capsulitis, is a painful and frustrating shoulder condition that causes progressive stiffness and restricted movement. While it often resolves over time, frozen shoulder can significantly impact daily life, work, sleep, and independence if not properly managed. Early assessment, education, and physiotherapy support can make a meaningful difference throughout recovery.
Frozen Shoulder
Frozen Shoulder
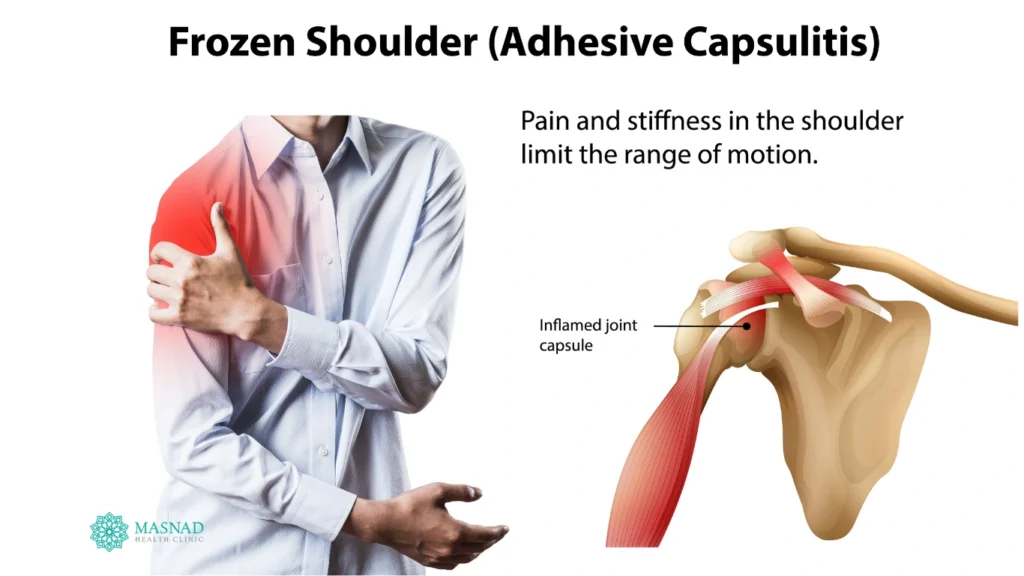
What Is Frozen Shoulder?
Frozen shoulder is a condition that affects the joint capsule of the shoulder. The capsule becomes inflamed, thickened, and tight, leading to pain and a gradual loss of shoulder movement in all directions.
Frozen shoulder is classified into two types:
- Primary Frozen Shoulder – develops without a clear cause
- Secondary Frozen Shoulder – occurs following injury, surgery, or prolonged shoulder immobilisation
Unlike many shoulder injuries, frozen shoulder follows a predictable pattern of progression and is considered a self-limiting condition, meaning it usually improves over time. However, without appropriate care, recovery can take 2-3 years and may not always be complete.
Stages of Frozen Shoulder
Frozen shoulder typically progresses through three stages:
1. Freezing Stage
This is the most painful phase.
- Gradual onset of shoulder pain
- Pain at rest and at night
- Increasing stiffness
- Painful and restricted movements, especially:
- Lifting the arm away from the body
- Rotating the arm outward
Daily tasks such as dressing, grooming, and reaching overhead become difficult.
2. Frozen Stage
Pain may start to reduce, but stiffness worsens.
- Less constant pain
- Significant restriction of movement
- Functional limitations remain high
- Activities such as lifting, reaching behind the back, and sleeping on the affected side remain difficult
3. Thawing Stage
Movement slowly begins to return.
- Pain continues to ease
- Gradual improvement in range of motion
- Strength and shoulder control start to improve
Recovery during this phase can take many months.
Common Symptoms of Frozen Shoulder
Symptoms can vary between individuals but commonly include:
- Deep aching pain in the shoulder
- Gradual loss of shoulder movement
- Difficulty with daily activities (dressing, grooming, driving)
- Pain when reaching overhead or behind the back
- Night pain and disturbed sleep
- Shoulder stiffness that does not improve with rest
Frozen shoulder often feels different from muscle strains or rotator cuff injuries, with global stiffness in all directions being a key feature.
Who Is at Risk?
Frozen shoulder most commonly affects:
- People aged 40 years and over
- Women more than men
Risk factors include:
- Diabetes
- Thyroid disorders
- Prolonged shoulder immobilisation
- Shoulder trauma or surgery
- Stroke
- Heart disease
- Autoimmune conditions
People with diabetes are more likely to develop frozen shoulder and may experience longer recovery times.
How Is Frozen Shoulder Diagnosed?
Frozen shoulder can mimic other shoulder conditions in its early stages, such as:
- Rotator cuff tears
- Shoulder impingement
- Labral injuries
Your physiotherapist will perform a thorough clinical assessment to rule out other causes of shoulder pain. Imaging such as X-rays or ultrasound may be used to exclude other conditions, but frozen shoulder is primarily a clinical diagnosis.
How Physiotherapy Can Help
Although frozen shoulder often resolves naturally, physiotherapy plays a crucial role in pain management, education, and restoring function.
During the Freezing and Frozen Stages:
Physiotherapy focuses on:
- Pain relief strategies
- Gentle mobility exercises within tolerance
- Reducing muscle guarding and tension
- Advice on posture, activity modification, and sleep positioning
- Education and reassurance about the condition and recovery timeline
Aggressive stretching is not recommended during early stages, as it can worsen pain.
During the Thawing Stage:
As pain settles, physiotherapy shifts towards:
- Gradual restoration of shoulder range of motion
- Strengthening exercises for the shoulder and shoulder blade
- Improving movement control and coordination
- Safe return to work, sport, and daily activities
Support and guidance throughout each stage are essential, as frozen shoulder can be emotionally and physically challenging.
Can Frozen Shoulder Be Prevented?
Frozen shoulder cannot always be prevented, particularly in primary cases. However, early movement and appropriate rehabilitation following shoulder injury or surgery can reduce the risk of secondary frozen shoulder.
Why Choose Masnad Health Clinic?
At Masnad Health Clinic, we understand how limiting frozen shoulder can be.
- Experienced physiotherapists trained in complex shoulder conditions
- Individualised treatment plans tailored to each stage of recovery
- Evidence-based physiotherapy approaches
- Clear education and reassurance throughout the process
- Focus on restoring confidence, movement, and function
We work closely with you to manage pain, maintain function, and support your recovery at every stage.
Conclusion
Frozen shoulder can be painful, restrictive, and slow to recover, but with the right support, most people regain meaningful shoulder function. Early assessment, stage-appropriate physiotherapy, and professional guidance can significantly reduce discomfort and help you navigate recovery with confidence.
For all your frozen shoulder concerns, feel free to call us at 02 9793 8840 or Book an Appointment Today.
FAQ
Typically 12–36 months, depending on severity and individual factors.
Yes, but recovery can be prolonged without physiotherapy support.
Yes, when guided appropriately and matched to the stage of the condition.
Recurrence is uncommon but possible, especially in people with diabetes.
Surgery is rarely required and usually only considered in severe, persistent cases.

New Client Offer - 10% OFF
Are you in pain? Not sure if we can help you?
Book your initial appointment and receive 10% off any service!