Ankylosing Spondylitis: Understanding, Managing, and Supporting Your Spine
Ankylosing Spondylitis (AS) is a form of inflammatory arthritis that primarily affects the spine, leading to pain, stiffness, and reduced mobility over time. While it can be a lifelong condition, understanding how it works and knowing how physiotherapy can help makes a significant difference in maintaining function and quality of life.
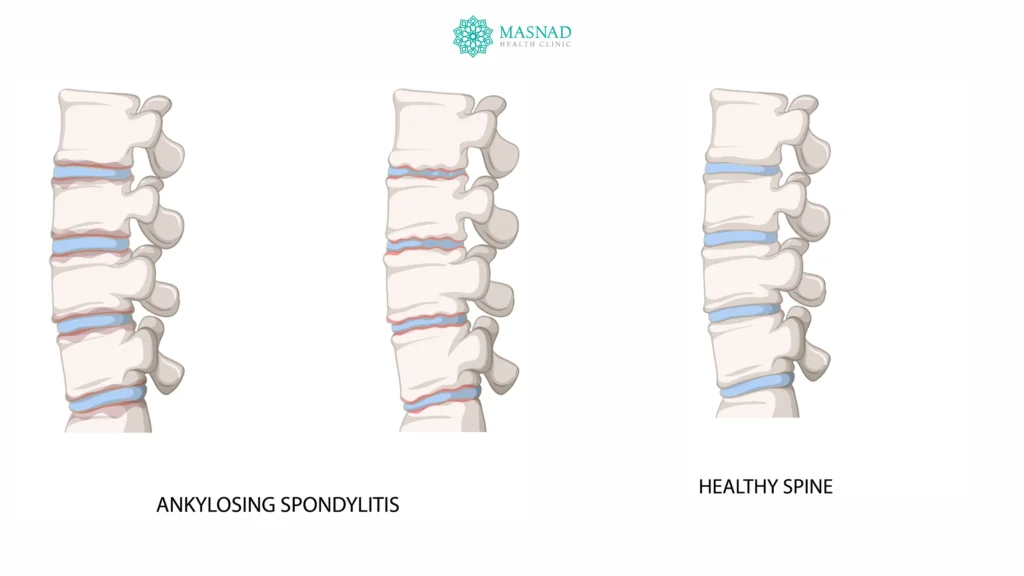
What is Ankylosing Spondylitis?
Ankylosing Spondylitis is an autoimmune condition where inflammation targets the spinal joints and ligaments. Over time, this inflammation can lead to hardening and fusion of spinal segments, often resulting in a forward-flexed posture.
Early symptoms usually include:
- Pain and stiffness in the lower back, particularly around the sacroiliac joints
- Discomfort after periods of rest, especially in the morning
- Flare-ups of pain followed by periods of relative relief
As AS progresses, it can affect other parts of the body, including the hips, shoulders, hands, feet, and ribs. Some people may also experience related issues such as irritable bowel symptoms or eye inflammation.
Causes and Risk Factors
The exact cause of AS is not fully understood, but several factors are known to contribute:
- Genetics: Certain genes increase susceptibility to AS.
- Age & Gender: Symptoms often begin between 17-45 years, and men are more frequently affected than women.
- Environmental factors: Chronic stress or repeated gastrointestinal infections may play a role.
While these factors increase the risk, the condition’s progression and severity vary widely between individuals.
Signs and Symptoms
The hallmark features of AS include:
- Intermittent or chronic back pain
- Progressive stiffness in the spine and joints
- Symptoms that improve with movement and worsen with rest
- Flare-ups and periods of remission
- Possible involvement of tendons, ligaments, and ribs, causing pain in the hands, feet, or chest
In severe cases, AS can lead to limited spinal mobility, difficulty breathing due to rib cage stiffness, and reduced overall function.
How Physiotherapy Can Help
Physiotherapy plays a key role in managing Ankylosing Spondylitis and slowing functional decline. Goals of treatment include:
- Pain management during flare-ups – Gentle exercises, posture support, and manual therapy can help reduce discomfort.
- Maintaining spinal mobility – Stretching and mobilisation exercises improve flexibility in the spine and chest.
- Strengthening surrounding muscles – Targeted exercises for the back, hips, shoulders, and limbs help maintain joint support.
- Improving posture and breathing – Exercises focusing on the thoracic region support rib expansion and proper spinal alignment.
Consistent physiotherapy has been shown to improve posture, reduce stiffness, and enhance quality of life for people living with AS.
Daily Strategies for People with AS
In addition to physiotherapy, lifestyle strategies can help manage symptoms:
- Maintain an active lifestyle with regular low-impact exercise, such as swimming or walking.
- Use heat therapy or gentle stretching to relieve stiffness, particularly in the morning.
- Incorporate breathing exercises to maintain chest expansion.
- Prioritise sleep and rest to support recovery and reduce inflammation.
How Masnad Health Clinic Can Support You
At Masnad Health Clinic, our physiotherapists provide individualised care for people with Ankylosing Spondylitis:
- Assess spinal posture, movement, and joint involvement
- Design tailored exercise programs to maintain mobility and strength
- Offer guidance for managing flare-ups and daily activity
- Collaborate with your medical team to support medication or specialist care
With ongoing support, most people with AS can maintain independence, manage pain, and preserve spinal function.
Book an Appointment
If you have Ankylosing Spondylitis or suspect you might, early physiotherapy assessment can help manage symptoms and maintain mobility.
Book your appointment online today
Or call us on (02) 9793 8840
FAQs
Yes, regular physiotherapy and exercise maintain spinal mobility, reduce stiffness, and improve posture.
No, symptoms vary widely. Some experience mild, occasional discomfort, while others have frequent, severe flare-ups.
Yes. Besides the spine, it may involve hips, shoulders, ribs, hands, feet, and eyes.
Gentle movement, stretching, heat therapy, and guidance from a physiotherapist can help manage pain.
In advanced cases, fusion can occur, but early and consistent management slows progression and preserves function.

