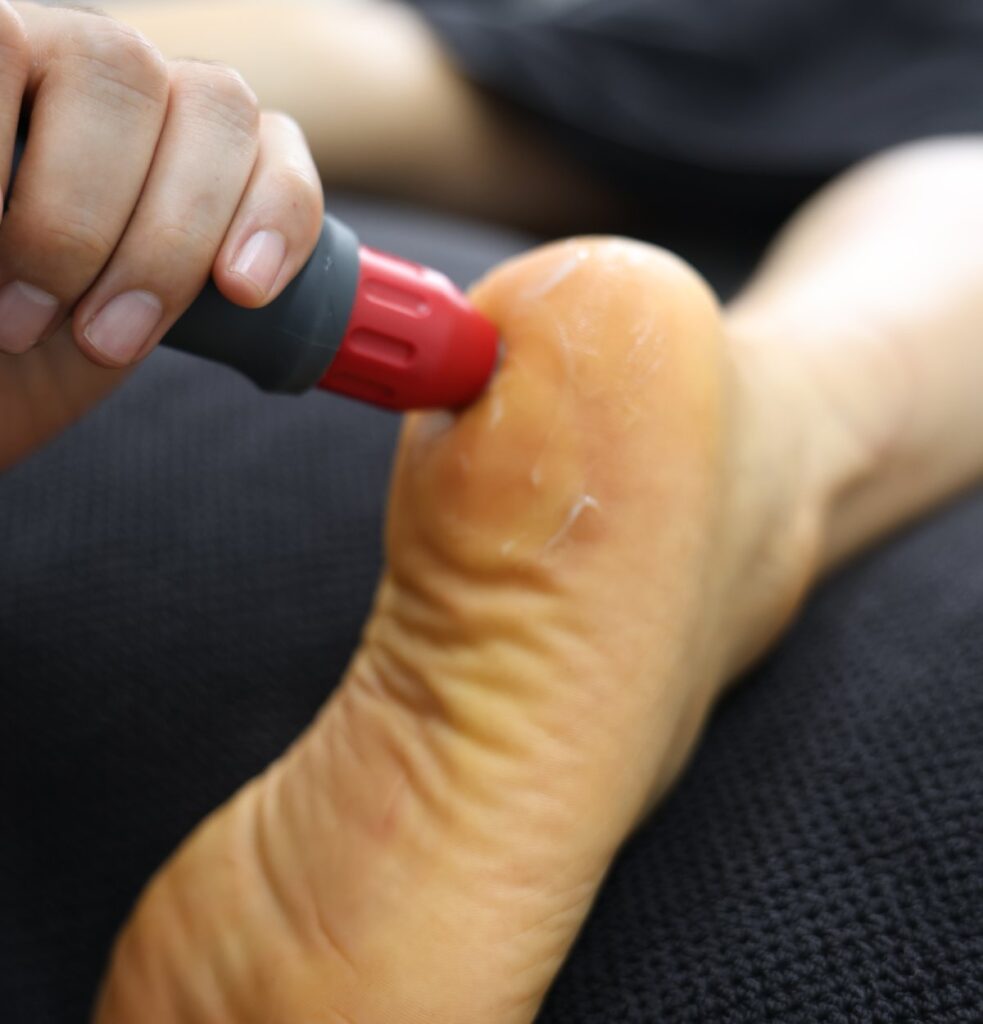
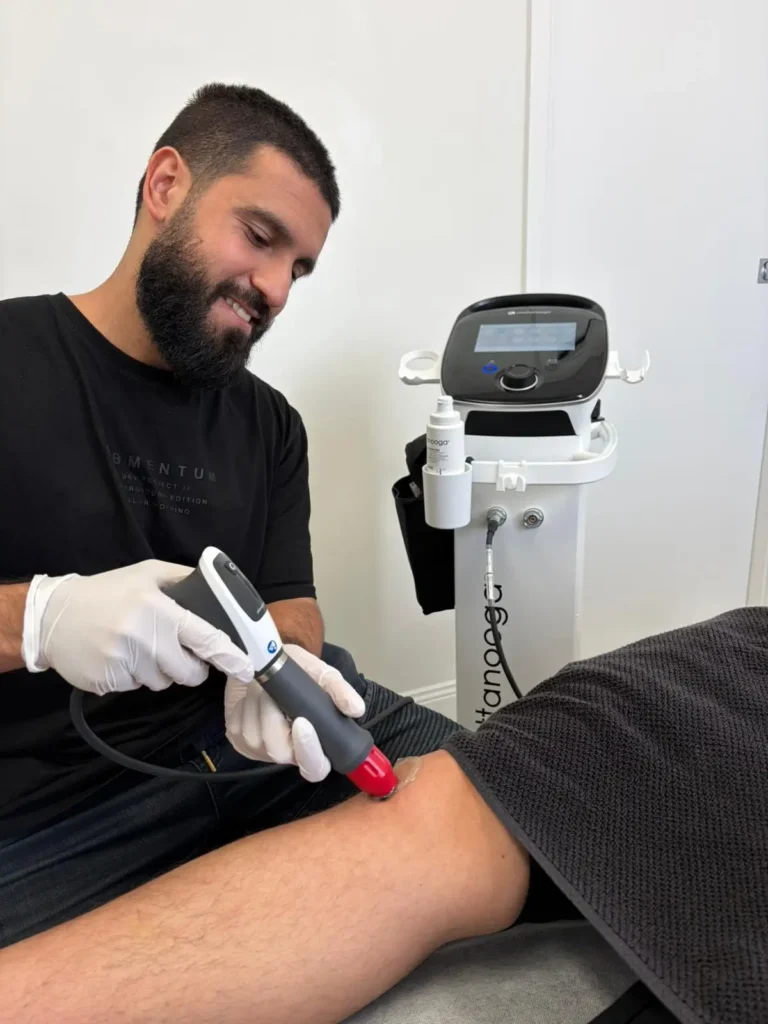
Joint replacement surgery is often described as one of the most significant advances in modern healthcare. For many people living with severe joint pain and limited mobility, it can offer the chance to move more freely and return to daily activities with less discomfort.
However, deciding whether or not to have a joint replacement is rarely straightforward. It is a personal decision that depends on many factors, including pain levels, function, lifestyle, overall health, and response to conservative care. Understanding what joint replacement surgery can and cannot offer is an important step before moving toward a surgical consultation.
Understanding Joint Replacement Surgery
Joint replacement surgery involves removing damaged parts of a joint and replacing them with artificial components designed to restore movement and reduce pain. The most common procedures involve the hip and knee, particularly in people with arthritis-related joint changes.
Over recent decades, advances in surgical techniques, implant design, and rehabilitation have significantly improved outcomes. As a result, many people experience meaningful improvements in pain and function after surgery. That said, surgery is not always the first or only option.
Arthritis Does Not Always Mean Surgery
Hearing the word “arthritis” can be confronting. Many people assume that once arthritis is present, pain is permanent and surgery is inevitable. In reality, arthritis is only one part of a much bigger picture.
Pain is complex and rarely caused by a single factor. While joint degeneration becomes more common with age, many people have visible arthritic changes on scans without experiencing significant pain or limitation. Conversely, some people with minimal structural change can experience high levels of discomfort.
Before considering surgery, it is often worth exploring non-surgical options such as:
- Physiotherapy assessment and treatment
- Strengthening and conditioning programs
- Improving joint mechanics and movement patterns
- Manual therapy and guided exercise
- Education around pain and activity modification
For many individuals, these approaches can significantly improve symptoms and delay or even remove the need for surgery.
When Pain and Function Become Limiting
Joint replacement is usually considered when pain and stiffness begin to significantly interfere with daily life. This may include:
- Difficulty walking or standing for extended periods
- Trouble with stairs, sitting, or getting up from chairs
- Sleep disruption due to joint pain
- Reduced ability to exercise or stay active
- Ongoing symptoms despite appropriate conservative care
The decision is not based on pain alone. Function, quality of life, and personal goals all play an important role.
The Importance of Pre-Surgical Strength and Fitness
If joint replacement surgery becomes a likely option, physical preparation is essential. Research consistently shows that people who are stronger and fitter before surgery tend to recover more effectively afterwards.
Pre-surgical rehabilitation may help by:
- Improving muscle strength around the joint
- Maintaining cardiovascular fitness
- Reducing stiffness and swelling
- Supporting better movement patterns
- Preparing the body for post-operative rehabilitation
Timing also matters. Waiting until pain becomes unbearable can lead to reduced strength, decreased activity levels, and added stress on other joints. In some cases, earlier intervention allows for better overall outcomes.
Understanding Risks and Expectations
While joint replacement surgery has high success rates, no surgery is without risk. It is important to understand both the potential benefits and the limitations.
Possible considerations include:
- Surgical risks such as infection or complications
- Ongoing pain or stiffness after surgery
- Time required for rehabilitation and recovery
- Temporary limitations on work and daily activities
Most people improve after joint replacement, but recovery is a process rather than an instant fix. Having realistic expectations and a clear rehabilitation plan can make a significant difference to long-term outcomes.
Exploring Conservative Care Before Surgery
For many people, conservative management remains an effective option, even when arthritis is present. Physiotherapy can help by addressing contributing factors such as muscle weakness, joint stiffness, poor movement patterns, and nervous system sensitivity.
A trial of non-surgical care is often recommended before surgery to:
- Assess how much symptoms can improve without an operation
- Build strength and confidence in movement
- Provide clarity about whether surgery is truly needed
Even if surgery is ultimately chosen, this preparation can improve post-operative recovery.
Making an Informed Decision
Deciding whether to have a joint replacement is highly individual. There is no universal right or wrong answer. The best decision is one that is informed, supported, and aligned with your personal goals and lifestyle.
Open discussions with qualified health professionals can help you understand:
- The source of your pain
- Available treatment options
- Likely outcomes with and without surgery
- The role of rehabilitation before and after surgery
Final Notes
Joint replacement surgery can be life-changing for some people, but it is not always the first step. Exploring conservative care, building strength, and understanding your options can help you make a confident and informed decision.
If you are unsure whether joint replacement is right for you, consider speaking with a qualified physiotherapist who can assess your movement, discuss non-surgical options, and guide you through the decision-making process based on your individual needs.
Call now to book your physiotherapy appointment: (02) 9793 8840
Why Choose Masnad Health Clinic
Masnad Health Clinic focuses on helping people make informed decisions about their health through personalised, evidence-based care. Rather than taking a one-size-fits-all approach, the team looks at how movement, strength, lifestyle, and pain sensitivity all interact to influence joint health and recovery.
With a multidisciplinary team working together, care is tailored to support both non-surgical management and pre- or post-surgical rehabilitation when needed. Emphasis is placed on education, guided exercise, and practical strategies that help you move with confidence and manage symptoms effectively over the long term.
The approach is collaborative, supportive, and centred on helping you understand your options so you can choose the path that best suits your needs and goals.
FAQs
No. Many people manage symptoms effectively with non-surgical care.
Yes. Improving strength and movement can reduce pain and improve function.
In most cases, yes. Conservative care is often recommended first.
Yes. Better strength and fitness before surgery often lead to smoother recovery.
Recovery varies, but improvement typically continues over several months.